There is an endemic nutritional deficiency likely to be affecting a large proportion of modern populations but especially Australians, including the next generation of Australian children. Reducing IQs, sapping vitality, expanding waistlines and impeding reproductive health… can all this really be influenced by one nutrient?
Well, given the average modern diet, lifestyle and environment, you would be forgiven for asking ‘which one?’ But in truth, beyond Vitamin D and the Omega 3 essential fatty acids (some of our other most notably universal nutritional deficiencies), it is Iodine that should be sitting squarely in our sights as a primary ‘first port of call’ for any nutritional assessment in Australia.
This becomes increasingly significant when we consider that, of all the things to be deficient in, Iodine, as well as Omega 3 and Vitamin D, each facilitate some of the most universal and integral functions within the body. Impacting multiple hormones (both steroidal and metabolic), the integrity of the nervous system (both cognitive and sensory) and ultimately the metabolism of every cell in the body (both directly and indirectly).
Iodine
Iodine is a large, volatile Halogen that is utilised in the body in BOTH its natural forms (as Iodine and Iodide) and therefore, due to apparently poor biological inter-conversion; we often need to acquire it in both of these forms. Iodine and Iodide are concentrated to the highest degree in the tissues that require it the most.
Over 30% of our total body store of this essential element is concentrated within the Thyroid gland, which has been estimated to retain up to 50mg alone (preferring the Iodide form), whilst the rest is distributed throughout the breasts (preferring the Iodine form), skin, gastric mucosa and visceral organs and can equate to a total Iodine/Iodide body store as high as 1,500mg across all tissues in very replete individuals. This incidentally makes it quite difficult to accurately assess overall body Iodine status through current conventional and non-invasive means.
Interestingly, whilst the nervous system is not the primary location of Iodine concentration in the body, the importance of Iodine to healthy cognitive development is perhaps one of Iodine’s greatest significance to our health.
The Deficiency
Beyond the above-mentioned capacity for the body to retain Iodine, it is estimated that about 30% of the world’s population is Iodine deficient. That number is supposed to be steadily falling in certain parts of the world, however due to the age and quality of the agricultural topsoil in Australia, limited seafood/seaweed consumption, increased consumption of processed food (that no longer contains sufficient traces of iodine from changes to uses of salt fortification and dairy sanitation), Australia now stands as one of the most markedly Iodine deficient nations in the world (and almost exclusively so out of those in the developed world!).
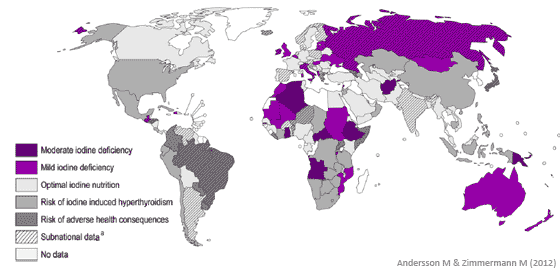
Severity of National Iodine Deficiency
(based on median I urine levels in school-age children)

The Effects
Given the factors described above, consideration of Iodine deficiency is particularly relevant to the clinical presentations of Fibrocystic Breast, other female reproductive Cysts/Nodules, Fatigue, resistant Weight Gain, Thyroid disease of any nature, Cognitive Impairment and especially during Pregnancy.
With regards to IQ, moderate to severe iodine deficiency during pregnancy has been shown to result in a reduced average IQ in the newborn during their early childhood. This is related to the fact that during the first two trimesters of pregnancy, the fetus is totally dependent on the mothers T4 production for healthy brain development. Even a small decrease in the serum T4 level during pregnancy, (from either iodine deficiency or other reasons for thyroid disease), is an important risk factor for impaired psychomotor development in infants.
Iodine & Halides: The Double Whammy
The other half of the Iodine deficiency story is the suppression of what little Iodine is actualy present by the other Halides (i.e. Fluoride and Bromide). Being Halogens just like Iodine these Halides can wreak havoc on Iodine utilisation and therefore its retention in the body and also have their own subsequent toxicities associated with them that therefore can make them particularly detrimental in situations of autoimmunity (of all descriptions, but especially thyroid related) and thus adequate avoidance of these Halides is clearly as equally important as iodine replenishment in the resolution of Iodine deficiency and its associated conditions.
Most notably, minimising systemic Fluoride exposure may be particularly crucial for optimising IQ and neurological function, for reasons beyond simply it’s Iodine displacement, after over 36 multi-age human studies have linked Fluoride to neurological impairments and reductions in IQ itself.
How Do We Determine Iodine Status?
Whilst ‘Skin Patch Testing’ is quite entrenched in popular wisdom as an appropriate means of determining iodine status, it has been shown for over 80 years to be more reflective of merely dermal oxidation conditions and ambient humidity (with close to 90% of the Iodine evaporating from the skin within 72 hours and only 1-4% making its way to the blood stream, at no greater or reduced rate between different regions of more or less replete or even healthy skin), skin patch testing for Iodine is therefore completely unreliable as a tool for determining total body Iodine status.
As mentioned, the specificity of iodine concentration and utilisation throughout the body means a much more functional and in depth sampling method is needed. Namely, urine. Urine allows an insight into metabolic activity (from what was circulating in the blood) and therefore the current background Iodine exposure available to the body.
There is also the ability to measure Halides alongside Iodine levels within urine and gain an even more complete assessment of ‘Iodine Sufficiency’ by identifying what level of obstructions to Iodine might be present via the Halides also. This ‘functional’ assessment of Iodine status can assist in selecting appropriate sources of Iodine and determine the efficacy of overall replenishment/treatment regimes over time.
Replenishing Iodine
Minimum Recommended Daily Intakes for Iodine hover around 150mcg for adults and 220mcg for pregnant women (acknowledging that there is a greater need during this key time). However these numbers are determined from population studies seeking to simply alleviate goitre and by no means reflect total body optimisation doses. It has been determined that women intending to fall pregnant should aim to obtain at least 280mcg of Iodine from combined food and supplement sources in order to maintain the minimum urine levels of Iodine required to see a preventative benefit of cognitive impairment in their child.
The amount required to achieve true body sufficiency is likely to be somewhat greater than these baseline doses for many individuals, especially in Australia, and can only really be determined by appropriate urine testing. How much greater may just surprise you.
Note:
– It is recommended that you always consult a nutritionally trained healthcare professional before making any significant dietary changes or commencing any focussed dietary supplementation.
– Any regimen you adopt should be monitored at regular intervals for efficacy and prevention of any excessive and unnecessary treatments/supplementation.
– Elimination of the ‘toxic Halides’ (Fluoride and Bromide), will enhance and perhaps dictate your sucess in addressing any Iodine related concerns.
– Thyroid ‘sufficiency’ is determined by testing TSH, T4 and T3 – and in cases of Autoimmunity, also Thyroid Antibodies. Testing for changes in these is recommended during any Iodine replenishment program.
– Sometimes those with Iodine sensitivity or severe Grave’s disease may not be able to handle increased sources of Iodine (even when Iodine deficient) and thus specific strategies will need be employed for these individuals with the guidance of their healthcare practitioner.
The Importance of Cofactors
Tyrosine
For Proper Thyroid (and Adrenal) Health, Tyrosine is the most important ‘substrate’ to include with Iodine to ensure its appropriate utilisation. However excessive amounts of Tyrosine (>3g per day) have been shown to suppress the conversion of T4 to the more active T3 (which may be useful in Hyperthyroidism but would be counterproductive in Hypothyroidism). So appropriately combined levels of Iodine and Tyrosine should always be maintained.
Selenium
Additionally, whenever Iodine intake is increased, appropriate inclusion of Selenium should ensure proper utilisation of Iodine and the conversion of T4 to T3 (however too much can be just as bad as too little).
Zinc also supports the conversion of T4 to T3, however the Australian population is not necessarily as universally deficient in Zinc (although it is not uncommon either). So it is perhaps advisable to assess both Zinc and Selenium status with your nutritional healthcare practitioner during any Thyroid/Iodine related treatment.
Vitamin A
Vitamin A is the often forgotten, but is perhaps the most crucial nutritional consideration after Iodine sufficiency for proper Thyroid hormone function in the body. In fact, whilst zinc is indeed important for the conversion of T4 to T3, supplementation with Zinc has been shown to not be as effective as supplementing with Vitamin A in raising T3 and Free T3 in those with hypothyroid presentation.
This is because the true ‘active’ retinoid forms of Vitamin A (such as those found in Liver and Cod Liver Oil) are required to support the action of thyroid receptors around the body, (through a multitude of shared interactions with retinoid receptors).
This is demonstrated in regions of the world where Iodine sufficiency HAS been confirmed (such as Sudan), yet goitre still remains endemic in those regions due to the prevalence of pronounced Vitamin A deficiencies.
If we then consider how inefficiently most individuals convert beta-carotene to vitamin A (from sources such as carrots), the importance of ‘preformed’ Vitamin A (e.g. retinol) supply to maintain optimum thyroid function becomes evident.
Vitamin D & DHA
On the topic of optimising cognitive function, it is important to also note the importance of both Vitamin D and DHA to brain health, particularly during early neurological development, along with the prevalence of their deficiency in Australia.
DHA has been well established as an essential nutrient to both brain structure and function, with increases in newborn brain weight, and subsequently childhood IQ, seen in mothers achieving higher levels of DHA during pregnancy.
Equally, Vitamin D receptors have been shown to appear within a wide variety of brain tissues during early fetal development, increasing nerve growth in the brain when activated. This effect also extends to adulthood where Vitamin D metabolically supports areas of the brain involved in planning, processing of information, and the formation of new memories. The National Institutes of Mental Health has recently concluded that it is vital that mothers get enough vitamin D during pregnancy in order for their baby’s brain to develop properly.
Conclusions
Addressing some of these common and basic deficiences, through potentially simple diet and lifestyle modicications, stands to support individual health on an extremely fundemental level. One that underlies many other health priorities, both as we age, and especially also in early life, to support the next generation of Australian mothers and children.
To Your Best,
Warren

